The opportunity to expand Medicaid to more low-income adults has opened the door to health coverage for millions of people who may never have had insurance before or who may have been uninsured for a long time. Many have pressing health needs that they have not been able to address because, without coverage, they could not afford to see a doctor or obtain necessary medications. Among the states that have not expanded Medicaid, the median eligibility threshold for parents with dependent children is just 45% of the federal poverty line. That means a parent in a family of three with income of more than $8,905 a year in 2015 could have too much money to qualify for Medicaid . Generally, in states that have not yet expanded, non-elderly adults not raising children do not qualify for Medicaid at all unless they have a disability.
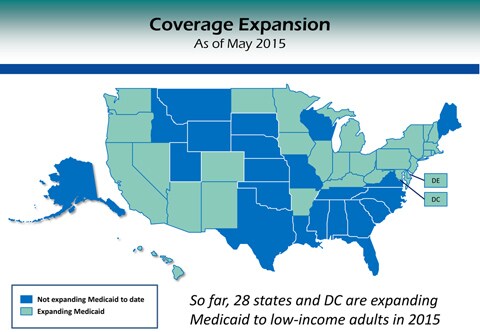
To date, 28 states and the District of Columbia have expanded their Medicaid programs to cover more low-income adults.
According to the latest CMS enrollment report (PDF, 1.22 MB), between October 2013 when the initial Marketplace open enrollment period began, and March 2015, over 12.2 million additional individuals are enrolled in Medicaid and CHIP. Among states that had implemented the Medicaid expansion and were covering newly eligible adults in March 2015, Medicaid and CHIP enrollment rose by approximately 28.1% compared to the July-September 2013 baseline period. States that had not expanded Medicaid reported an increase of about 8.6% over the same period.
CMS is offering links/charts for informational purposes only, facts should not be construed as an endorsement of the organization's programs or activities

